Healthcare Innovation Sandboxes: Fostering Innovation at the Intersection of Self-Interest and Collaboration
Posted by David Richards on October 5, 2023, 2:05 PM EDT

Innovation in the complex landscape of healthcare is often stymied by diverse challenges ranging from stakeholder coordination, to stringent regulations, to operational complexity and stretched budgets.
This blog outlines how live systems we’ve brought up with partners, in markets both domestic and overseas, to address real world needs, can be used as laboratories or for market trialing by others. To in effect, use our production environments that have existing users and resources as “sandboxes” for introducing or testing products and services, eliminating the need of carrying the entire burden of such a system.
Finally, the core concept underlying all of these systems is that of Consumer -Controlled Direct Engagement. A term we've coined because it highlights the central notion that patients must control the process and be actively engaged in it. Not merely vessels being carried along the journey.
Collaboration done well catalyzes innovation broadly
Innovation rarely thrives in a vacuum. More commonly it occurs in defined market places (“communities”) and when certain conditions converge. Key among these being:
- Large economic interests are at play: When there’s money to be made, and especially when there’s lots it, people and organizations show up. Capitalism and self-interest work.
- There are unmet needs: When there are large gaps in the marketplace or problems to be solved, new solutions inevitably emerge. Solutions are sometimes for payment, other times provided charitably or as a social good.
- There is commonality of tools and methods: Common methods, tools and processes remove friction. Less friction saves costs, removes barriers to trial and error, all of which drive opportunity that everyone benefits from.
- New participants are welcome: Assuming good behavior, new participants following their own self-interest are welcomed. They add numbers, bring new skill sets and add capacity. Metcalfe’s law at work.
Game changing examples of collaboration done well
Within the context of the above consider Linux, the Web/Internet and Git; they are real-world exemplars of massive innovations that addressed significant economic interests and market gaps in their respective domains. While each has its own unique story, Git is particularly relevant to this discussion on healthcare innovation and “sandboxes”.
Initiated by Linus Torvalds, Git revolutionized software development by creating a distributed sandbox for code. This open-source project streamlined the software development process, enabling frictionless collaboration among a global community of developers, akin to the healthcare ecosystem sandboxes we’re suggesting. Git provides a controlled environment where innovation can be tested, refined, and deployed without affecting the broader ecosystem. It embodies the principles of economic self-interest, streamlined processes, and evolving business models, making it a fitting example for those of us working to innovate in healthcare.
Healthcare innovation is difficult even in the best of circumstances
Using Git as a conceptual starting point it’s important, if not obvious, to note that a healthcare innovation sandbox requires a much more expansive notion. Why? Because healthcare is a unique, incredibly complex beast fraught with challenges that are absent in other sectors. Thus it requires a much broader ecosystem of connected people, processes, protocols and products to be effective.
One of the most significant hurdles for healthcare innovators is the sheer number of stakeholders involved in healthcare delivery. Accordingly, coordinating trial projects can be akin to herding cats with each stakeholder needing to be on-boarded and their own interests and concerns addressed.
Adding to the complexity is the local nature of healthcare. Unlike digital products that can be launched globally with the click of a button, healthcare services must be tailored to specific communities and conditions, making logistics a constant challenge. This is further complicated by stringent regulations like HIPAA which can make even the simplest pilot project expensive if one needs to initiate it from scratch.
Financial constraints are another roadblock and particularly so because product development is generally so expensive. Often budgets have been stretched thin just as innovators near “the finish line” making go-to-market strategies difficult to undertake. Related, as certain expertise like forming corporate development relationships frequently resides only with the CEO, functional bottlenecks exist.
Our sandboxes: collaborative ecosystems for innovators
Our sandboxes address many of the challenges noted above because what we’re calling a sandbox (from a newcomer’s perspective) is in reality an existing, live environment in which we and subsets of partners are doing real work. Participants and stakeholders variously include consumers, patients, clinicians, non- and for-profit organizations and increasingly new and emerging products and services companies.
Consider for example Lynchburg Cares. It focuses on the needs of Lynchburg, Virginia. Lynchburg Cares was initially founded by us (Open Health Innovations), the Lighthouse, a free clinic serving the community’s most needy and MoveUP, a software enabled micro-transportation provider . Along the way, however, a broad range of other organizations have been engaged including the department of health, the local drug court, a leading automobile dealer, local schools and universities and all manner of individuals including pediatric cancer patients. In addition, as this is being written discussions are progressing with innovators ranging from AI solutions, to next-generation blood screening, to mental health providers.
As a second example consider an earlier stage system in Soweto, the huge, iconic township outside of Johannesburg, South Africa. Its collaborators naturally are a very different mix. In addition to us there are clinicians from Stanford Medical School and the Chris Hani Baragwanath Hospital (the largest hospital in Africa), MoveUP, A Better Africa, a leading educational portal based in Johannesburg and a range of local service providers.
What’s in a sandbox
Because every implementation (e.g. Lynchburg and Soweto) is different due to addressing different market needs, the possible capabilities available to newcomers of the sandbox vary to some degree.
Graphic 1: Lynchburg Cares components
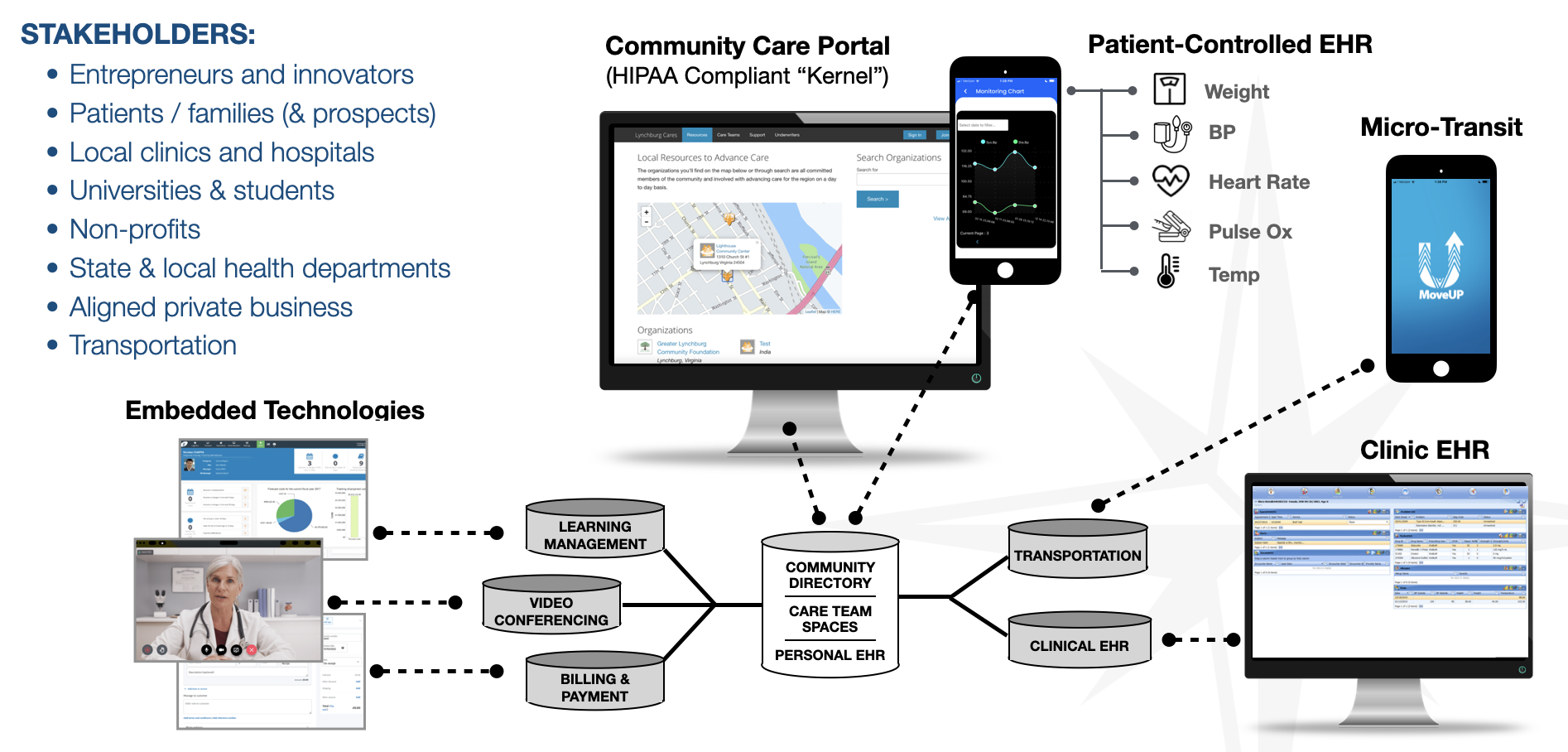
The graphic above articulates some of the resources commonly available. At the core of the network from a technology perspective is what we consider the “Kernel”. It is a robust, permissions driven, HIPAA compliant collaborative portal that houses a Community Directory, Care Team Spaces, Personal EHR (Electronic Health Records) and whose API allows other servers (and thus applications) to be integrated with it.
The Kernel communicates with a range of specialized servers and with new ones easily added through a standard, RESTful API. The MoveUp Server in Lynchburg, for instance, powers a Micro-Transit app similar to Uber and is used to provide rides for patients in need beginning originally with pediatric oncology. There's also a Clinical EHR application tailored for free clinics and embedded application servers that handle learning management, video conferencing and billing & payment.
Finally, because healthcare innovation exists for and is driven by people, sandboxes most importantly involve individuals, their skill sets, needs and the different roles they play. Such stakeholders typically range from entrepreneurial leaders and experts, to patients and their families, local clinics, hospitals, universities, students, non-profits, and local health departments.
A few rules: open platforms and emerging patient-centric protocols
In general our systems (and thus as sandboxes) are open platforms and not limited to a single focus or geography. They are usually lead by a small group of motivated individuals or organizations and are operational in diverse locations like Lynchburg and as far afield as Soweto and Lagos, Nigeria. Specialized communites also exist to address specific challenges such as Autism and Mental Health in the U.S., and Education in Africa and also welcome newcomers to use them, where appropriate, as a sandbox.
Within these environments adherence to a simple set of protocols is both crucial and we believe fair. For example, guidelines from practical frameworks like Institutional Review Boards (IRB) provide an ethical foundation. Additionally, we are collaborating with a group of for- and non-profit partners in advancing two protocols we believe are missing and needed. One we’ve tentatively labelled the PDO (Patient Data Ownership) and the other the PCA (Patient Care Access). Subsequent blogs and white papers will be released on these.
